7 Reasons Why Medical Practices are Turning Toward AI Front Desk Agents
Seven common reasons why medical practices adopt AI—from tackling high call volume, reducing staff burnout, and helping practices...

You’ve probably seen the stat: missed calls cost the average medical practice six figures a year. That number gets cited frequently across the healthcare industry.
Whether this figure is correct or not, such estimates miss the point.
They calculate the cost of one missed appointment. The patient called, nobody picked up, the appointment didn’t happen. Lost revenue. End of story.
Except that’s just the beginning of the story.
What actually happens after a missed call is a chain reaction that compounds the damage—from the missed appointment, to the patient who walks away, to the wasted marketing dollars you spent acquiring them in the first place. It’s hard to see because no practice gets a notification that says “a patient just booked with a competitor instead.”
If you’re a practice manager, office administrator, or physician owner who suspects your phones might be costing you more than you realize, this article walks through that chain, gives you a framework to estimate the cost for your specific practice, and shows what it looks like when the problem is eliminated entirely.
Industry estimates suggest that no-shows cost the U.S. healthcare system roughly $150 billion annually. At the practice level, MGMA research puts the damage at around $150,000 per physician per year in some models.
Those are big numbers. But they primarily measure appointments that were scheduled and not kept. They’re less likely to capture the patient who called, never got through, and booked with a competitor—because that interaction was never logged in the first place.
And they almost certainly don’t factor in the marketing dollars that brought that patient to your phone, or the years of follow-up visits, procedures, and referrals that walked out the door with them.
The missed appointment is just the most visible cost. Underneath it sits a chain of compounding losses that starts the moment nobody picks up.
Here’s the sequence that plays out behind the scenes:
Maybe the front desk is checking in a patient. Maybe it’s a Tuesday at 9:15am and three lines are ringing at once. Maybe it’s 7pm and the office closed two hours ago. Whatever the reason—the call goes unanswered or to voicemail.
Most don’t. Voicemail introduces uncertainty. The patient doesn’t know when (or whether) someone will call back. They needed something resolved—an appointment, a refill—and voicemail doesn’t resolve anything.
They still need care. They pull up search results and call the next practice. If that practice picks up, the appointment is booked. Your revenue just became someone else’s.
A 2024 Accenture consumer survey, cited by the American Hospital Association, found that about 1 in 5 consumers switched providers in the past year. Nearly 90% who switched said the organization was hard to do business with—citing issues like bad experiences with administrative staff and digital tools that didn’t meet their needs.
If that patient found you through a paid ad, a referral, or SEO, you already spent money getting them to call. That investment returns nothing when the call isn’t answered.

Here’s a simple framework to estimate what missed calls are costing your specific practice:
(Daily calls) × (miss rate) × (% that are appointment-related) × (avg. revenue per visit) × (working days per month) = monthly revenue leakage
The variables will differ by specialty. A primary care visit might average $150–$250. A specialist visit might be $300–$500+. Your miss rate depends on staffing, call volume patterns, and whether you have any coverage after hours.
And not every missed call is a bookable appointment—many are about refills, billing, or general questions—so a realistic estimate of the appointment-related share matters too.
Here’s what the math looks like for three types of practices, assuming roughly 30% of missed calls were appointment-related:
Practice type |
Daily calls |
Estimated miss rate |
Missed calls/day |
Appointment-related (~30%) |
Avg. visit revenue |
Monthly loss (20 days) |
Solo practice |
40 |
25% |
10 |
3 |
$200 |
$12,000 |
3-physician group |
100 |
20% |
20 |
6 |
$200 |
$24,000 |
5-physician group |
175 |
15% |
26 |
8 |
$200 |
$32,000 |
These are illustrative examples—your actual numbers will vary by specialty, practice size, and payer mix. The point is to plug in your own figures and see what the leakage looks like.
For the solo practice in this example, that works out to roughly $144,000 per year—and these figures still only capture the direct visit revenue. They don’t include follow-up visits, procedures, lab work, imaging, or the lifetime value of a patient who might have stayed with your practice for years.
Missed calls during business hours get most of the attention. But there’s another gap that’s easy to overlook: the hours when no one is there at all.
Many practices have limited or no phone coverage during lunch, after 5pm, on weekends, and on holidays. Yet patients don’t stop needing care on a schedule. And with 71% of medical groups still reporting fewer than 1 in 4 patients scheduling digitally, most patient interactions still happen by phone—including outside office hours.
Jimmy Kallikadan, CEO of Health + Glow Primary Care and Med Spa in Tampa, saw this firsthand. In just their second month using Talkie.ai, the AI agent created nearly 200 patient cases—and over a third of them came in during off hours.
We would have missed out on all those patients. What if there were important cases? We had the opportunity to capture all those patient inquiries and then get back to them when we were back in the office.
During the holidays, the gap gets even wider. A mid-sized primary care clinic in Texas that uses Talkie.ai saw this between December 24 and January 4: the AI front desk agent handled 246 after-hours requests, created 149 patient cases in the EHR, and scheduled or rescheduled 35 appointments—all while the staff was off.
If you’ve read this far and your first instinct is “we need to hire another receptionist,” consider the math.
The Bureau of Labor Statistics reports that the median annual pay for secretaries and administrative assistants—a category that includes medical front desk staff—was $47,460 in May 2024. And that new hire still can’t answer calls at 8pm on a Wednesday, still can’t handle three simultaneous conversations, and still needs lunch breaks, sick days, and vacations.
The problem isn’t that front desk staff are failing. Walk into any medical practice and you’ll see people working hard—checking patients in, verifying insurance, responding to providers, handling walk-ins—all while the phone rings. Hiring more people is an expensive way to partially address a structural issue.
And the phone experience matters more than most practices realize. A peer-reviewed study published in the American Journal of Managed Care found that longer phone wait times at VHA medical facilities were associated with lower patient perceptions of their ability to access urgent care—even when actual appointment wait times hadn’t changed.
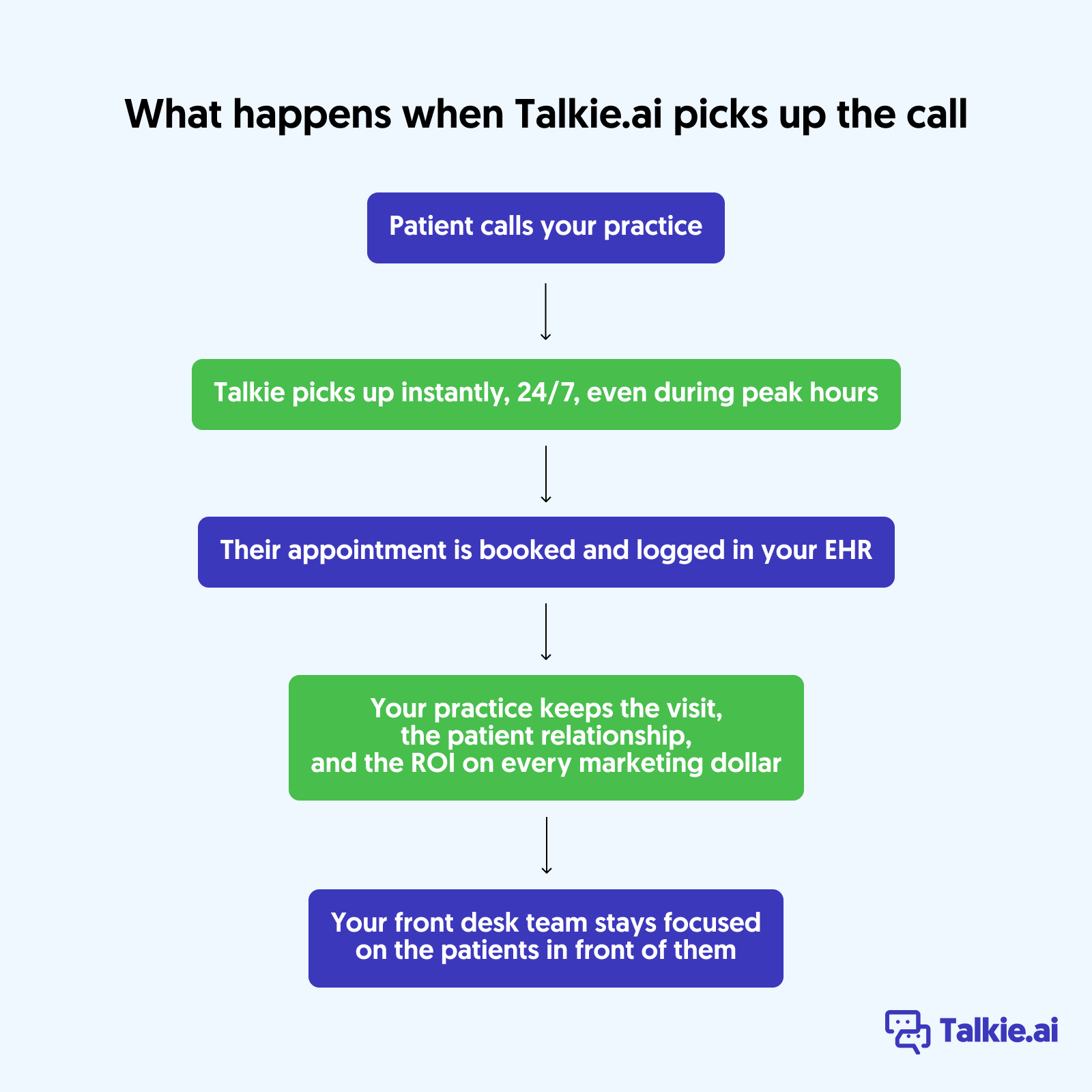
Let’s map back to the chain from earlier.
Talkie picks up every call instantly, 24/7. It handles unlimited concurrent calls, so there’s no hold time, no busy signal, and no voicemail during peak surges.
Talkie can schedule appointments, answer FAQs, process prescription refill requests, or route urgent calls to the right person. When a message for the provider is the right outcome, Talkie takes it—but the message is captured in your EHR with full context, not sitting in a voicemail box.
Talkie completes interactions after hours—including booking appointments directly into your EHR—so patients get what they need when they call, not the next business day.
When a new patient calls and there’s no chart yet, Talkie creates one in real-time by collecting key information and logging it directly in the EHR. The patient can schedule immediately.
By handling the repetitive calls, Talkie gives your front desk team back the capacity for work that requires a human: complex patient questions, in-person care, and provider support.
One multi-location urology practice saw the impact within days of deploying Talkie. In the first week, voicemails dropped by 50%. The AI now serves 3,500+ unique patients per month, handles up to 11 concurrent calls at peak times, and the practice reduced call center staffing needs by 1 FTE.
As one physician told us:
Working with the team at Talkie.ai has been a truly smooth experience! We’ve already noticed a significant difference since implementing their virtual front desk, effectively eliminating the issue of missed calls.
And one detail that surprised several of our clients: patient adoption among older demographics is strong. One practice found that patients in their mid-60s were regularly using the AI to schedule appointments—a population they had expected to resist the technology.
Your front desk staff are doing their best inside a structure that wasn’t designed for the volume and complexity of modern patient communication.
Every unanswered ring is a patient making a decision. And the data tells us that most of them won’t call back.
How much does a missed call actually cost a medical practice?
It depends on your specialty and payer mix. Depending on the type of visit, a typical office appointment might generate anywhere from $150 to $500+. But the direct appointment value is only the tip of the iceberg. The real cost includes the patient’s lifetime value—follow-up visits, procedures, referrals—which can run into the thousands over several years.
What percentage of calls do medical practices typically miss?
It varies widely depending on practice size, staffing, and phone infrastructure. A peer-reviewed study in AJMC found that even large VHA medical facilities with dedicated call center staff had meaningful call abandonment rates. Smaller, single-receptionist practices likely experience higher miss rates during peak hours, lunch, and after hours. That said, most practices don’t track this closely enough to know their actual number.
Why don’t patients leave voicemails?
Patients calling a medical practice usually need something resolved—an appointment, a refill, a question answered. Voicemail introduces uncertainty: they don’t know when they’ll hear back or whether their message was received. For many patients, it’s faster and easier to call the next practice on their list than to wait for a callback.
How does Talkie.ai handle missed calls differently than a traditional answering service?
Traditional answering services take messages. Talkie.ai takes action—scheduling appointments directly into your EHR, answering patient FAQs, processing prescription refill requests, creating new patient charts, and routing urgent calls to on-call providers. Many of the patient’s needs are resolved on the spot, not queued for a callback.
Will patients actually talk to an AI on the phone?
Yes. One Talkie.ai client was surprised to find that even patients in their mid-60s regularly used the AI assistant to schedule appointments. Adoption tends to be driven by convenience: if the AI resolves the patient’s need quickly and naturally, most patients prefer that experience to waiting on hold or leaving a voicemail. Talkie supports multiple languages, which further increases adoption in diverse patient populations.
Does Talkie.ai integrate with EHR systems?
Yes. Talkie.ai integrates with popular EHR systems: athenahealth, ModMed EMA, Elation Health, and eMedicalPractice. Appointments, patient charts, messages, and refill requests are logged directly in your system—so your staff sees everything in their normal workflow without needing a separate tool.
Want to see what 100% call coverage looks like for your practice?

Seven common reasons why medical practices adopt AI—from tackling high call volume, reducing staff burnout, and helping practices...

Looking to add an AI assistant to your medical practice? This buyer’s guide outlines key questions to ask vendors before making a...